National Skin Centre gets $10m grant to study eczema, reduce rates of severe disease in Singapore
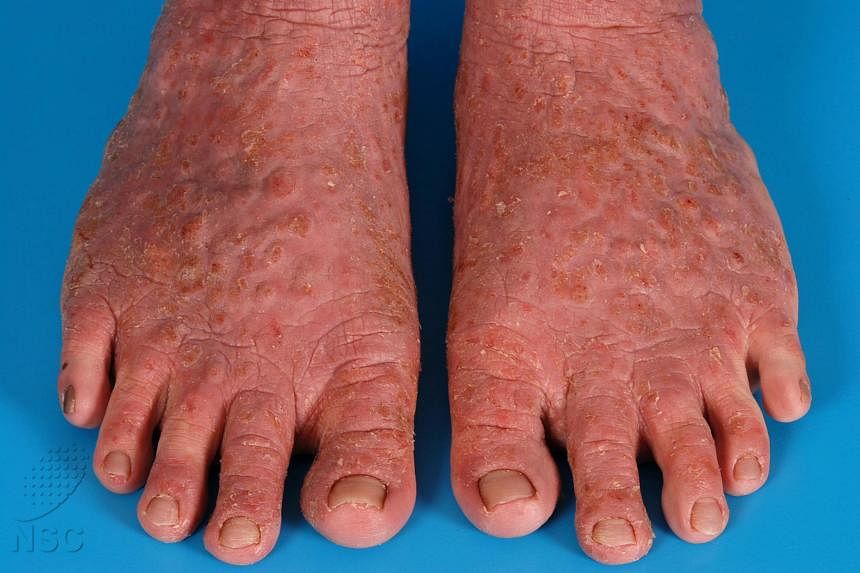
SINGAPORE – It is the itch that will not stop, affecting one in five children and one in 10 adults in Singapore.
Atopic dermatitis, often known simply as eczema, is a chronic condition that causes inflammation, redness and irritation of the skin. As it is the most prevalent skin problem here, researchers want to unravel how it develops among Asians and find new ways of treating it.
They are also looking into tailoring treatment to each patient, given how costly new therapies are.
To fight eczema, the researchers at the National Skin Centre (NSC) will use a new war chest of nearly $10 million.
NSC received the grant in May – the first to be allocated to skin research by the National Medical Research Council under its Open Fund-Large Collaborative Grant, which aims to advance human health and wellness and create economic value for Singaporeans.
The money will fund the Atopic Dermatitis Research Programme for Patients (Adept), a four-year study.
Atopic dermatitis is the most common form of eczema. It usually begins in childhood, but anyone can get it at any age.
There is no single cause. It occurs due to a deficiency in skin barrier function and an overactive immune system. Genetic and environmental factors, gut microbiome and stress also play a role in it. People with the disease have a higher chance of developing allergic conditions like food allergies, asthma and allergic rhinitis.
NSC handled more than 14,000 new eczema cases in the year ending March 31, 2023.
However, there remain many gaps in the understanding of the condition.
“At the moment, genetic studies revealed genetic factors that could only explain 20 per cent to 30 per cent of the risk of atopic dermatitis,” said Dr Yew Yik Weng, the consultant in charge of NSC’s Eczema Clinic.
As there is a difference between eczema in Asians and the type in Caucasians, the researchers will focus on getting a better grasp of the disease in Asians. This will enable them to better translate any therapeutic results of overseas clinical trials of new therapies, Dr Yew said.
Recent years have seen the rapid development of new treatments, with many more on the horizon, spelling hope for those with moderate to severe forms of the disease who have skin that may ooze fluid, crust or bleed. They have widespread inflamed skin that is challenging to treat, unlike those with mild eczema that can be treated with emollients and topical steroids.
If patients do not respond to topical therapies, light therapy may be offered, followed by systemic treatments such as conventional immunosuppressants, biologic drugs or Jak inhibitors.
Currently, Dupilumab is the world’s first biologic drug approved for moderate to severe atopic eczema, and the only targeted therapy approved in Singapore.
Biologics, which are drugs made from biological sources like animal or plant cells, have revolutionised the treatment of eczema. Unlike traditional drugs that affect the whole body, biologics target only a specific component of the immune response that is driving the disease.
Dupilumab is a safe and effective treatment that has been approved here for children aged six months and older, and around 60 per cent of people will see a 75 per cent improvement in their condition, said Dr Yew.
However, it is costly, requires ongoing treatment, and does not work on all patients. Typically given by injection every fortnight, it costs nearly $1,000 per jab, or about $24,000 a year.
“If we can predict at the first injection whether the patient will respond (to the drug) or not, then we can better tailor treatments for patients, so that they don’t keep going for this expensive treatment (if it does not work),” said Professor Steven Thng, the corresponding principal investigator of Adept. He is also chief dermatologist at the Skin Research Institute of Singapore and the medical director of the Translational Research Office at the National Healthcare Group.
“Despite the high prevalence and significant personal and social costs of atopic dermatitis, there has been a lack of innovation in therapeutics, particularly for severe cases, and research in this area has been globally underfunded,” said Prof Thng.
There is a newer class of drugs approved for eczema, known as Jak (Janus Kinase) inhibitors, which are oral medications that are typically taken once a day.
These cost $6,000 to $10,000 a year, and have a higher efficacy rate than biologic therapy. However, they suppress the body’s immune system and may have potentially serious side effects, such as cancer and heart attacks, though these are rare.
There are other biologic and oral medication therapies in the pipeline. Some of the new biologics are undergoing phase three global clinical trials on safety and effectivenessin Singapore, and could be approved here in the years to come.
Dr Yew said a second, and even a third, biologic drug may be available in Singapore in 2025, but will likely be costly.
Eczema is the leading condition treated at NSC. It said the total number of cases has remained stable since 2019, but the proportion of moderate to severe cases has risen over the years.
Such cases can total about 1,000 to 1,200 a year, and the centre has had to increase the number of clinic rooms catering to these patients, said Dr Yew.
Adept aims to reduce the cases of serious eczema by 30 per cent and overall eczema cases by 10 per cent by 2027, according to NSC.
Prof Thng told The Straits Times that they will use non-invasive imaging techniques that NSC has developed in the project. One of the techniques is done with a locally patented imaging device to predict progression of the disease based on the chemical composition of the skin.
This will possibly make NSC the first in the world to use imaging technologies to study eczema so that therapy can be tailored for every individual, he said.
A second imaging device will be used to study the 3D structure of the skin to quantify the degree of the inflammation and determine if a treatment is working, he added.
Among the things they seek to understand is how obesity increases the risk of severe eczema, as they have noted that obesity is linked to the severity of eczema.
“Once we can understand how fats affect inflammation, we can theoretically intervene at the right pathway to prevent the worsening of eczema, so that they don’t progress from mild to severe, needing the more expensive or more dangerous medicine,” said Prof Thng.
Dr Yew, who is also the deputy head of NSC’s research division and one of Adept’s principal investigators, said he is assembling a group of 1,000 adult patients aged between 21 and 84, and 250 patients below the age of 18 for the study.
NSC will collaborate with A*Star, the Skin Research Institute of Singapore, NUS, NTU’s Lee Kong Chian School of Medicine, and the National University Hospital’s paediatrics department.
Said Prog Thng: “We are not doing what other people are doing. We are looking specifically at the Asian type of eczema, at (the link between) obesity and eczema, and at imaging so that we can better individualise therapy for patients.”
He added: “We want the public, or at least those who suffer from eczema, to have some hope that there are things going on... and hopefully, there are new ways to treat their eczema so that they don’t have to suffer so much.”
